Introduction: Why PRP Preparation Quality Matters
In orthobiologics, platelet-rich plasma preparation continues to grow in use. However, not all PRP is the same.
In fact, the way a PRP preparation system separates cells can directly affect PRP composition.
One key factor is the presence of neutrophils, a type of white blood cell. While neutrophils support immune defense, they may also influence inflammation and tissue response.
Therefore, clinicians are paying closer attention to leukocyte content in PRP preparation.
What Is Platelet-Rich Plasma (PRP)?
Platelet-rich plasma is an autologous biologic preparation derived from a patient’s own blood.
Clinicians produce PRP using a PRP preparation system and centrifugation.
Standard platelet-rich plasma preparation steps:
• collect a blood sample
• centrifuge the sample
• separate blood layers
• isolate platelet-rich plasma
The final PRP contains concentrated platelets and signaling proteins. Because of this, researchers continue to study platelet-rich plasma preparation across many specialties.
Neutrophils in PRP: A Complex Role
Neutrophils are part of the body’s natural immune response.
First, they respond quickly to injury. Then, they release enzymes and reactive molecules to clear damaged tissue.
However, in platelet-rich plasma preparation, high neutrophil levels may affect the biological environment.
How Neutrophils May Influence PRP Composition
1. Tissue Breakdown
Neutrophils release enzymes that can break down structural proteins such as collagen.
As a result, this activity may affect tissue environments, especially in cartilage and bone.
2. Oxidative Stress
Neutrophils produce reactive oxygen species (ROS).
Consequently, these molecules may contribute to oxidative stress, which can affect cellular structures.
3. Prolonged Inflammatory Signaling
Neutrophils release inflammatory mediators.
Over time, this may prolong inflammatory signaling in certain conditions.
4. Growth Factor Interaction
Platelets release growth factors that are widely studied in regenerative medicine.
However, neutrophil activity may influence the local environment where these signaling proteins act.
Leukocyte-Rich vs Leukocyte-Poor PRP
Because of these differences, researchers often compare:
Leukocyte-Rich PRP (LR-PRP)
• contains higher levels of white blood cells
• includes more neutrophils
• may create a more inflammatory environment
Leukocyte-Poor PRP (LP-PRP)
• reduced white blood cell content
• lower neutrophil levels
• designed to support a different cellular profile
As a result, many clinicians evaluate leukocyte-poor PRP preparation systems when reviewing technology options.
How PRP Preparation Systems Influence Cell Separation
Not all PRP preparation systems use the same design.
In fact, system technology plays a key role in:
• platelet concentration
• leukocyte separation
• red blood cell removal
• workflow consistency
Therefore, clinicians often compare system specifications when selecting a platelet-rich plasma preparation system.
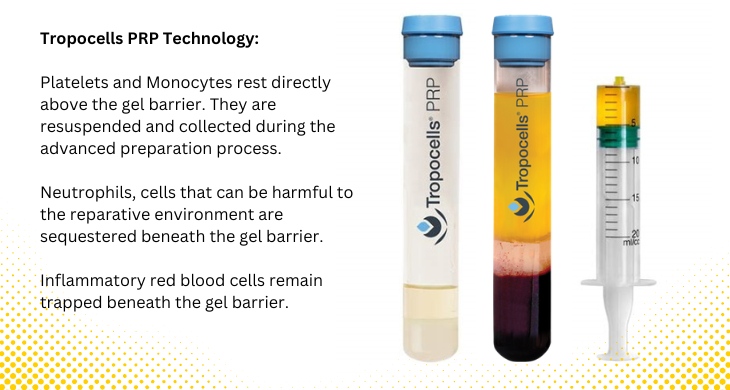
Gel Separator Technology in PRP Preparation
Modern systems may use gel separator technology to improve cell separation.
How gel separator PRP tubes work:
First, the blood sample enters the tube. Next, centrifugation separates components by density. Then, a gel barrier forms between layers.
As a result, the system may:
• separate platelet-rich plasma from unwanted cells
• reduce neutrophil presence
• minimize red blood cell contamination
This approach supports more controlled platelet-rich plasma preparation.
Tropocells® PRP Preparation System Design
Systems such as Tropocells® PRP use gel separation and controlled centrifugation.
These systems are designed to:
• reduce neutrophil presence
• minimize red blood cells
• support consistent platelet concentration
• produce a reproducible preparation workflow
Because of this, clinicians often evaluate these systems when reviewing PRP preparation system performance.
Limitations of Buffy Coat PRP Systems
Older buffy coat PRP preparation systems use a different approach.
While they may produce high platelet concentrations, they often:
• retain higher neutrophil levels
• include more mixed cellular content
• create less controlled separation
As a result, newer systems focus on more selective cell separation.
Why PRP Composition Matters
Platelet dose remains an important factor in PRP research.
However, cellular composition also matters.
Specifically, clinicians often evaluate:
• platelet concentration
• leukocyte levels
• red blood cell content
• reproducibility of preparation
Therefore, understanding PRP preparation system design helps guide clinical decisions.
Conclusion
Platelet-rich plasma preparation continues to evolve.
While PRP contains beneficial platelet-derived components, the presence of neutrophils may influence the final preparation.
For this reason, many clinicians review:
• leukocyte content
• system design
• preparation protocols
As research advances, improved PRP preparation systems may support more consistent and controlled platelet-rich plasma preparation.
Regulatory Notice
Tropocells® systems are intended for the preparation of autologous platelet-rich plasma.
The clinical use of PRP is determined by the treating physician based on patient evaluation and professional judgment.
Statements regarding PRP composition reflect published scientific literature and are not intended to imply FDA-cleared indications for specific clinical outcomes.